Whilst hormonal symptoms can start before your period becomes irregular, not every unpleasant experience that is bothering you once you hit 40 can be attributed to your poor hormones. Understanding this can help set realistic expectations about the benefits of hormone therapy.
Perimenopause can be a perplexing stage in a woman’s life. It often arrives unannounced, making it challenging to pinpoint when it begins. Symptoms can be diverse, fluctuating, and not all are exclusively due to hormonal changes. Additionally, traditional hormonal treatments may not always be effective in addressing these issues.
Are you “peri”?
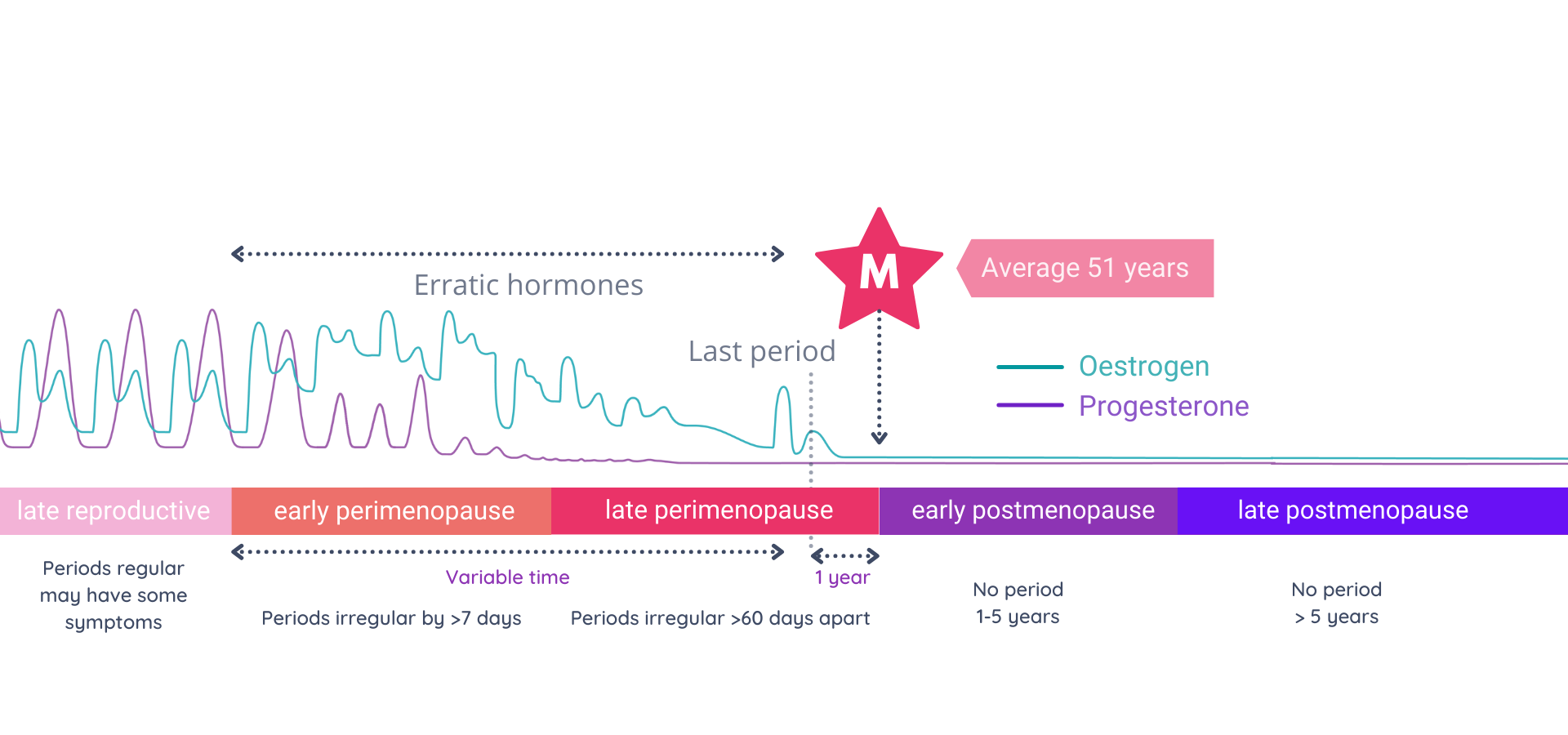
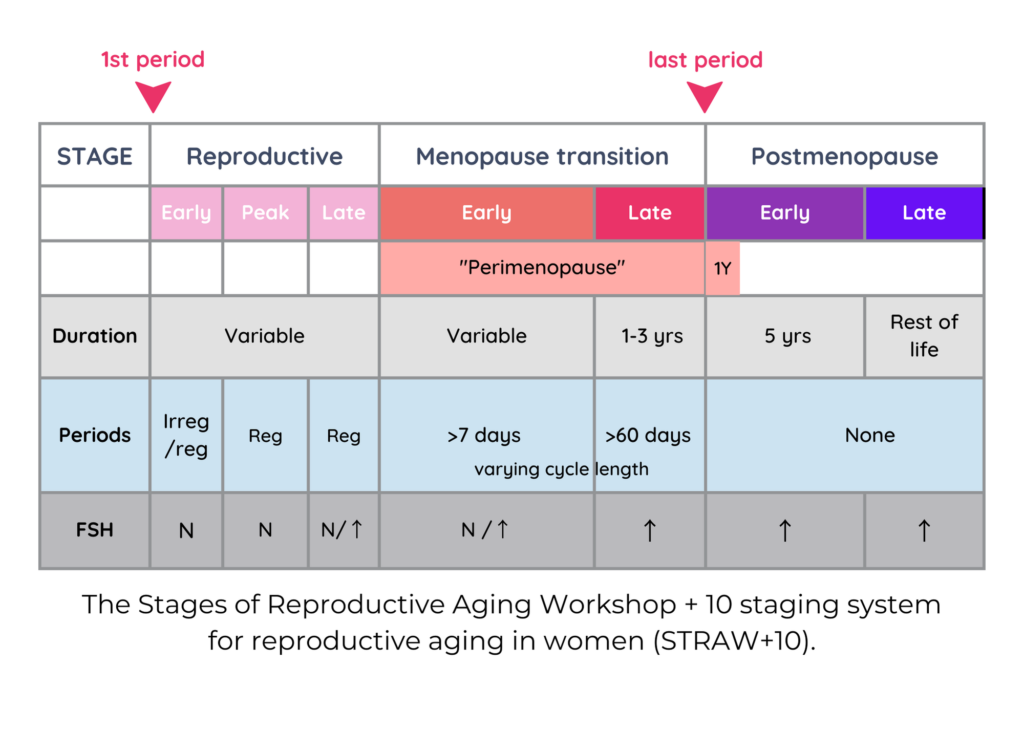
Perimenopause is generally understood as the transitional phase leading up to a woman’s final menstrual period. It can span over a decade and typically commences in one’s early 40s. While various formal definitions exist, the widely accepted one is known as the STRAW+10 classification. This categorises early perimenopause as the phase when your otherwise regular menstrual cycle deviates by more than seven days from its routine. Late perimenopause is characterised by cycles extending up to 60 days beyond the usual pattern, and it continues until 12 months after your last period.
Recognising symptoms
Symptoms of hormonal changes can manifest even before your menstrual cycle becomes irregular. These symptoms may include headaches, mood disturbances, alterations in menstrual flow, changes in PMS symptoms, occasional hot flashes (often during your period), and breast tenderness. When these symptoms occur in a cluster, and especially when they appear in a cyclic fashion linked to your period, you can be more confident in attributing them to hormonal changes. Many women describe less typical symptoms which cannot be as confidently attributed to hormonal change, even more so when they are occurring without the more typical symptoms.
It is no wonder women feel frustrated and often report feeling dismissed by doctors when they present with bothersome but unusual symptoms. Many women have tried many supplements and herbal products but the reality is that addressing hormonal symptoms during late reproductive and early perimenopause can be quite challenging. In addition, not all of these bothersome symptoms may be hormonally related.
The stages (STRAW+10)
- Late Reproductive Stage: Your menstrual cycle is mostly regular but may exhibit changes. Anovulatory cycles start becoming more common – resulting in low progesterone in the second half of the cycle and leaving oestrogen unbalanced.
- Early Perimenopause: Your menstrual cycle deviates by more than 7 days from its usual timing. Flow is also likely to be altered, often heavier, and you experience more and more anovulatory cycles and hormonal imbalances.
- Late Perimenopause: Your period is 60 days or more out of its usual timing, with fewer ovulations and fluctuating oestrogen levels. Progesterone levels are generally low.
- Menopause: Defined as the absence of a period for 12 consecutive months. Both oestrogen and progesterone are now low but stabilised.
- Early Postmenopause: The next 4 years after menopause (or the 5 years after your last period).
- Late Postmenopause: From 5 years after your last period for the rest of your life!
(The STRAW+10 classification starts at the first period, but we have only included the relevant stages here.)
It’s important to note the variability in hormone levels and menstrual patterns throughout these phases. Treatment for symptoms should be tailored to their nature, severity, health background and the likely hormonal changes occurring.
Managing early hormonal symptoms
Managing symptoms during early perimenopause can be challenging. Ovarian function becomes erratic and there is no accurate way to measure it. Focusing on lifestyle factors, such as sleep, exercise, limiting alcohol, and a balanced diet, is a good starting point. Maintaining a healthy weight is also crucial, as it can impact the severity of symptoms in later menopausal transition stages.
Some options include using a combined birth control pill to override your natural cycle and alleviate symptoms. This solution is not recommended for women over 50, or over 35 who are also overweight, smoke, or have a history of blood clots. This can be a great solution for women needing contraception. Coming off the OCP requires planning as menopausal symptoms may rebound.
Progesterone, either in the second half of your cycle or daily, can also be tried. Combined hormone replacement therapy (HRT), including both oestrogen and progesterone, can be effective for some women, especially in late perimenopause. Often women try many treatment strategies before finding one that suits them.
For those dealing with heavy irregular bleeding, using progesterone in the second half of the month or a hormonal IUD can provide relief. The hormonal IUD is especially suitable for those who need contraception and can also offer endometrial protection if oestrogen therapy is initiated.
As you approach late perimenopause and menopause, when your ovaries are truly winding down, using hormone therapy to treat symptoms becomes much more predictable.
If you are trying to find answers to bothersome symptoms, and are feeling frustrated by the lack of clarity and effective solutions, be reassured that as time goes on, this will become easier!
NOTE – Many other medical conditions can mimick symptoms of perimenopause, including thyroid dysfunction. Please make sure you get your symptoms checked and exclude other causes.
THIS INFORMATION IS FOR GENERAL EDUCATIONAL PURPOSES ONLY AND DOES NOT CONSTITUTE MEDICAL ADVICE. PLEASE SEE YOUR HEALTH PROFESSIONAL FOR ADVICE THAT IS PERSONALISED TO YOU.
Key Take Aways
Hormonal symptoms can start before your period is irregular.
It can be difficult to manage hormonal symptoms when your hormones are erratic and unbalanced.
Perimenopause formally starts when your period is more than 7 days out of routine.
HRT becomes more effective as you approach the late perimenopause and menopause.






